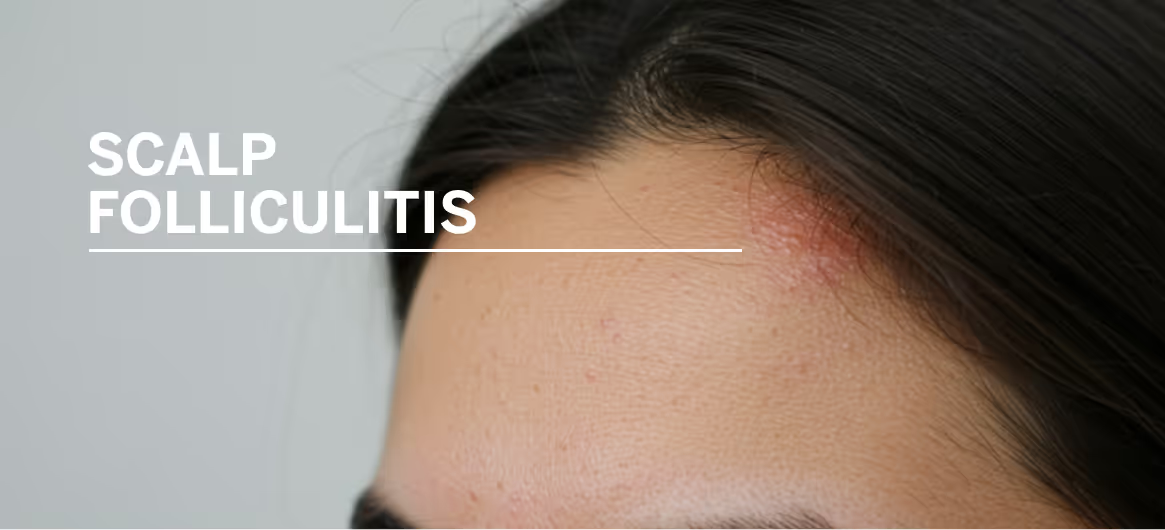
Those small, red bumps on your scalp that look like acne might actually be scalp folliculitis. This bacterial or fungal infection occurs when hair follicles become inflamed, causing itchy, sometimes painful pustules that can spread if left untreated.
Scalp folliculitis develops when bacteria, yeast, or other organisms enter damaged hair follicles. Common triggers include excessive sweating, tight hairstyles, dirty hair accessories, or certain hair products that clog pores.
The condition appears as clusters of small pimples around hair follicles, often accompanied by tenderness, burning sensations, or crusty sores that won't heal. Even though the condition is uncomfortable, most cases respond well to proper treatment and simple lifestyle changes.
Understanding how and why this inflammation develops is essential to managing and preventing flare-ups and protecting your hair and scalp long term.
With the right knowledge and a dermatologist’s guidance, you can identify triggers early, choose effective treatments, and maintain a healthier, calmer scalp.
What Is Scalp Folliculitis?
Scalp folliculitis is an inflammatory condition that affects the hair follicles on the scalp. It typically appears as small red or skin-colored bumps that may be tender, itchy, or filled with pus. These bumps often resemble acne and can cluster around individual follicles or form small patches.
The surrounding skin may look slightly swollen or irritated, and some areas can develop crusts as lesions heal. While the condition is usually mild, the inflammation can occasionally lead to more noticeable irritation or discomfort if not properly managed.
What Causes Scalp Folliculitis?
Scalp folliculitis can develop from several underlying triggers, with the most common being bacterial infection, particularly Staphylococcus aureus, which causes inflamed, pustular bumps around individual follicles.
Yeast overgrowth, especially Malassezia yeast, may produce more diffuse itching and redness with smaller, uniform bumps. Viral infections and mites such as Demodex are less common but can create similar inflammatory reactions.
Folliculitis may also result from friction or irritation caused by tight headwear, frequent shaving, heavy sweating, or occlusive hair products that trap heat and moisture around follicles.
In some cases, noninfectious inflammation, such as that seen with acneiform eruptions or certain medications, triggers follicle irritation without noticeable pus formation.
Understanding the specific cause helps guide appropriate treatment and reduce recurrence.
Signs and Symptoms of Scalp Folliculitis
Scalp folliculitis often begins with increased sensitivity or a mild burning sensation before visible lesions appear.
As inflammation develops, small papules or pustules form around follicles and may feel sore when touched. Some people experience noticeable itchiness that worsens with sweating or heat. In more active flare-ups, clusters of bumps can form, creating patchy areas of irritation.
The scalp may feel rough or uneven due to the raised lesions, and dried serum or crusting can occur as pustules rupture and heal.
Inflammatory cases may also produce a tight or tender feeling when combing or washing the hair, and scratching can lead to further irritation or secondary infection. Severe folliculitis creates deep, painful nodules that can lead to permanent hair loss if untreated.
Possible Complications
Complications of scalp folliculitis can vary depending on severity and duration.
Recurrent or untreated infections may spread, causing more extensive inflammation. Persistent episodes can lead to post-inflammatory hyperpigmentation or hypopigmentation, especially in darker skin tones.
Severe forms, such as acne necrotica, may result in crusted lesions that heal with pitted scars. In chronic or destructive cases, ongoing inflammation can damage follicles, leading to scarring alopecia and permanent hair loss if not addressed promptly.
Who Is Most at Risk for Developing Scalp Folliculitis?
People are more likely to develop scalp folliculitis if they have naturally oily skin, sweat heavily, or wear tight hats, helmets, or other head coverings that trap heat and moisture. Those with poor hygiene habits are at risk as well.
People who use occlusive hair products or shave their scalp regularly also face a higher risk due to increased friction and follicle irritation.
Those with diabetes, weakened immune systems, or underlying skin or scalp conditions, such as dermatitis or acne, may experience more frequent or severe episodes. Additionally, athletes and individuals in hot, humid environments are especially prone to flare-ups.
Treatment Options
Scalp folliculitis is highly manageable, and effective treatment depends on the underlying cause, severity, and how frequently flare-ups occur.
Both over-the-counter and prescription options can effectively manage symptoms when used correctly, and modifying the way you care for your scalp can help soothe discomfort and reduce the chances of reinfection.
Changes to Your Care Routine
A gentle, consistent routine can significantly reduce irritation and help follicles heal. Using lukewarm water when shampooing prevents additional inflammation, while warm compresses can soothe tenderness and encourage drainage of superficial pustules.
Switching to non-occlusive, fragrance-free hair products reduces the risk of clogging follicles. It’s also important to wash pillowcases, hats, combs, and brushes frequently to minimize bacteria or yeast buildup.
Avoiding tight headwear, harsh scrubbing, or frequent scalp shaving further reduces friction-related flare-ups.

Over-the-Counter Solutions
OTC treatments can support mild cases and complement prescription care. Antibacterial washes containing benzoyl peroxide help reduce bacterial load, while antifungal shampoos with ketoconazole, selenium sulfide, or zinc pyrithione target yeast-related folliculitis.
Products with salicylic acid or glycolic acid provide gentle exfoliation to prevent buildup around follicles. Hydrocortisone solutions may offer short-term relief from itching and inflammation, though they should be used sparingly.
Prescription Treatments
Dermatologists may prescribe oral or topical antibiotics when bacterial infection is confirmed or strongly suspected. For yeast-driven folliculitis, stronger antifungal shampoos or oral antifungal medications may be recommended.
In more inflammatory cases, topical corticosteroids or non-steroidal anti-inflammatory solutions help calm irritation. For chronic or recurrent episodes, oral medications such as doxycycline may be used for their anti-inflammatory benefits.
Severe variants such as acne necrotica or scarring folliculitis may require longer treatment courses, combination therapy, or advanced procedures to control inflammation and protect hair follicles.

Rethinking Your Daily Scalp Care Routine
A thoughtful daily scalp routine can make a meaningful difference in reducing inflammation and preventing future folliculitis flare-ups. Prioritizing gentle cleansing, consistent hygiene, and non-irritating products helps maintain a healthier scalp environment.
- Wash the scalp regularly with a mild, non-comedogenic shampoo.
- Use lukewarm water to avoid triggering additional irritation.
- Rinse thoroughly to prevent residue buildup around follicles.
- Choose lightweight, non-occlusive conditioners and styling products.
- Avoid tight hairstyles and headwear that trap heat or moisture.
- Disinfect combs, brushes, hats, and pillowcases frequently.
- Minimize scratching, aggressive scrubbing, and unnecessary scalp manipulation.
Prevention Strategies
Prevention strategies reduce the frequency and severity of scalp folliculitis outbreaks. Small changes can make the biggest difference in long-term management when implemented consistently.
Hygiene practices form the foundation of prevention. Wash hair regularly based on scalp oil production. Typically, washing every 1–3 days is recommended for most people.
Change bed linens weekly and pillowcases more frequently during active outbreaks. Disinfect hair tools after each use with 70% isopropyl alcohol. Keep fingernails short and clean to minimize bacterial transfer from scratching.
Environmental modifications reduce exposure to triggering factors. Install a shower filter if water quality seems to worsen symptoms.
Maintain indoor humidity between 30% and 50% to discourage bacterial growth, and choose breathable fabrics for head coverings instead of synthetic materials that trap moisture.
When To See a Dermatologist
You should see a dermatologist if your scalp folliculitis does not improve after several weeks of gentle care and OTC treatments or if symptoms worsen despite proper hygiene.
Persistent pain, widespread pustules, significant itching, fever, or areas that begin to crust, bleed, or scar warrant prompt evaluation.
A dermatologist can identify the exact cause, whether it’s bacterial, fungal, inflammatory, or mechanical, and prescribe targeted medications to prevent complications.
Seek care urgently if you notice patchy hair thinning, signs of spreading infection, or recurrent flare-ups that interfere with daily comfort.
Managing Scalp Folliculitis Successfully
Managing scalp folliculitis long-term involves paying close attention to what triggers your flare-ups and responding quickly when early signs appear.
Consistency is key. Gentle cleansing, thoughtful product choices, and routine hygiene help prevent inflammation from returning.
When symptoms do occur, early intervention with appropriate treatments can stop minor irritation from progressing into scarring or hair loss.
Most importantly, partnering with a dermatologist ensures you’re using the right strategies for your specific type of scalp folliculitis to keep your scalp healthier and more resilient over time.
Talk to a board-certified dermatologist to discuss your goals and find the solution that is best for you.
Frequently Asked Questions
What causes folliculitis on the scalp?
Scalp folliculitis occurs when hair follicles become inflamed, typically due to Staphylococcus aureus bacteria, yeast, friction, excessive sweating, or the use of occlusive hair products. Shaving, tight headwear, and poor scalp hygiene can also contribute to this condition.
How can I get rid of folliculitis on my scalp?
Improving scalp hygiene, using warm compresses, switching to non-occlusive products, and trying OTC antibacterial or antifungal shampoos can help. Persistent or severe cases often need prescription antibiotics, antifungals, or anti-inflammatory treatments from a dermatologist.
Is doxycycline good for folliculitis?
Yes, doxycycline is often prescribed for moderate to severe scalp folliculitis, especially when bacterial infection or inflammatory folliculitis is suspected. It helps reduce bacteria and inflammation, but it should only be used under a dermatologist’s guidance.
How long does it take to get rid of scalp folliculitis?
Mild cases of scalp folliculitis may improve within one to two weeks with proper care, while more stubborn or recurrent folliculitis can take several weeks and require prescription treatment. Chronic cases may need ongoing management to prevent flare-ups.
Is folliculitis contagious?
Scalp folliculitis itself isn’t typically contagious, but infections caused by bacteria or yeast can sometimes spread through shared items such as towels, hats, or pillowcases. Good hygiene and avoiding shared personal items help reduce transmission risk.
Can folliculitis cause permanent hair loss?
Most cases of scalp folliculitis don’t cause permanent hair loss, but severe or untreated folliculitis can damage follicles and lead to scarring alopecia, which is permanent. Prompt treatment helps reduce inflammation, prevent follicle destruction, and protect long-term hair growth.